

Let's simplify glucose management
Glucose monitoring is an essential part of patients’ diabetes management, but the pain and inconvenience of finger prick testing doesn’t make it easy1. By lowering the barriers to glucose monitoring, you can simplify diabetes management and enhance your patients’ care and outcomes.
Liberate patients from the hassles of glucose monitoring with the easy-to-use FreeStyle Libre 2 system2 – consistent accuracy3 for 14 days with optional alarms, eliminating routine finger pricks†

Sensor is water resistant in up to 1 metre (3 feet) of water. Do not immerse longer than 30 minutes.
In a survey of 12,000 FreeStyle Libre users*
Tap below to discover how the FreeStyle Libre 2 system is helping to improve diabetes care compared with finger prick testing5-9
- 2 in 3 diabetes patients skip finger prick testing5
- Finger pricks only provide snapshots of glucose levels6
- Finger prick testing can miss night-time hypos6
- >30% of diabetes patients miss their HbA1c target7
3 in 4 of surveyed users were scanning at least 8 times a day4
Finger prick testing causes anxiety in around 1 in 3 diabetes patients8, while two thirds find it invasive to their lives5. By enabling patients to monitor glucose easily and without the pain of finger prick testing, the FreeStyle Libre 2 system simplifies glucose monitoring and minimises disruption to patients’ lives†.

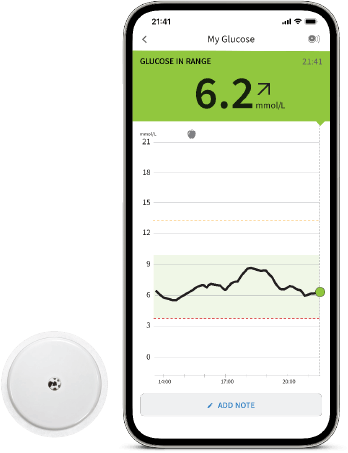
The 14-day FreeStyle Libre 2 system captures glucose readings every minute, day and night.
Frequently capturing glucose readings day and night, the FreeStyle Libre 2 system gives added dimension to glucose monitoring that makes it easier to spot hidden fluctuations and trendsΦ.

The FreeStyle Libre system reduced nocturnal hypoglycaemia by 52% compared to baseline (p=0.0002)9.
(Time spent with glucose <3.9 mmol/L 23:00-06:00 at 12 months9)
With the FreeStyle Libre 2 system the majority of patients chose to use the optional alarms to alert them if their glucose was too high or low (56%)4.

Since using the FreeStyle Libre system, around 60% of patients reported that they'd noticed improvements in HbA1c4
In our survey of over 12,000 people with diabetes, 59% of FreeStyle Libre users have seen better HbA1c results since starting the FreeStyle Libre system4.

When 85% (7907/9329) of surveyed users would never go back to routine finger pricks4, what does it tell you about the way your patients feel about glucose testing?
NICE updates guidance on flash glucose monitoring.
Learn about the future of glucose monitoring

Let’s simplify patients’ diabetes management with the FreeStyle Libre 2 system. To start taking positive steps towards managing diabetes, click here for webinars, podcasts and more.
*The survey of 13,088 patients was conducted on both FreeStyle Libre users and FreeStyle Libre
2
users.
† Finger pricks are required if glucose readings and alarms do not match symptoms
or expectations.
Φ For a complete glycaemic picture, users need to scan the sensor once
every 8 hours.
1. Vincze G, Barner JC, Lopez D. Factors associated with adherence to self-monitoring of blood glucose among persons with diabetes. Diabetes Educ. (2004);30(1):112-125. 2. Data on file, Abbott Diabetes Care, Inc. 3. Alva, S. et al. J Diabetes Sci Technol, (September 2020). http://doi.org/10.1177/1932296820958754. 4. Data on file 2022, Abbott Diabetes Care, Inc. 5. Wagner J, Malchoff C, Abbott G. Invasiveness as a barrier to self-monitoring of blood glucose in diabetes. Diabetes Technol Ther 2005;7(4):612–619. 6. Danne T, Nimri R, Battelino T, Bergenstal RM, et al. International consensus on use of continuous glucose monitoring. Diabetes care 2017;40:1631–1640. 7. NHS. National Diabetes Audit 2020-21 Quarterly report for England. Available at: https://digital.nhs.uk/data-and-information/publications/statistical/national-diabetes-audit [Last accessed July 2021] 8. Shlomowitz A, Feher MD. Anxiety associated with self monitoring of capillary blood glucose. Br J Diab Vasc Dis 2014;14:61. 9. Haak T, et al. Use of flash glucose-sensing technology for 12months as a replacement for blood glucose monitoring in insulin-treated type 2 diabetes. Diabetes Ther. 2017; 8:573–586. 10.National Institute of Health and Care Excellence (NICE). Thousands of people with diabetes set to benefit from real time information after updated NICE recommendations. Available at: https://www.nice.org.uk/news/article/thousands-of-people-with-diabetes-set-to-benefit-from-real-time-information-after-updated-nice-recommendations [Last accessed April 2022].
ADC-59351 v2.0 06/22